
Gentle Digestion: Simple Daily Habits for a H ..
May 08 - 2026
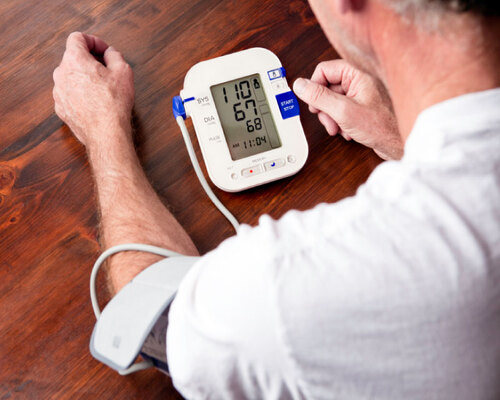
This article explores the substantial benefits of HBPM, offers a practical guide for getting started, and highlights how this simple practice can transform the management of hypertension.
Blood pressure is not a static number; it fluctuates throughout the day due to activity, stress, and environment. A single measurement in a clinic can be misleading, often influenced by "white-coat hypertension" (nervousness in a medical setting that elevates readings) or its reverse, "masked hypertension" (normal readings in the clinic but high readings elsewhere) .
HBPM addresses these issues by providing multiple readings in a person's natural environment over time.
The evidence supporting HBPM is robust. A 2025 systematic review and meta-analysis published in Hypertension Research, which included 65 studies, concluded that self-measurement of blood pressure at home resulted in a significantly greater reduction in blood pressure compared to usual care alone .
Furthermore, studies have consistently shown that home blood pressure is a better predictor of future cardiovascular events and target organ damage than office-based readings.Improved Accuracy and Diagnosis: By averaging multiple readings, HBPM provides a more reliable baseline, helping to correctly identify white-coat and masked hypertension.
To reap the full benefits of HBPM, it is crucial to use proper technique and equipment. Inaccurate measurements can be worse than no measurements at all.
Experts unanimously recommend using an automatic, or electronic, monitor that uses an upper-arm cuff.
Wrist and finger devices are generally less reliable unless measuring at the upper arm is not possible .Look for Validation: Ensure the device has been validated for accuracy by independent organizations such as the American Medical Association or the British Hypertension Society.
You can find lists of validated devices on websites like www.validatebp.org.
Accuracy depends on consistency and correct preparation.
Prepare Your Body: Avoid caffeine, tobacco, alcohol, and exercise for at least 30 minutes before measuring. Sit quietly for five minutes before you begin with your back supported, feet flat on the floor, and legs uncrossed .
The table below summarizes the key differences between blood pressure measurement methods .
| Measurement Method | Advantages | Limitations |
|---|---|---|
| Office BP Measurement | Professional equipment | Single data point; prone to white-coat effect; can misdiagnose |
| Ambulatory BP Monitoring (ABPM) | Gold standard; provides 24-hour data including nighttime readings | Expensive; impractical for long-term use; can be uncomfortable |
| Home BP Monitoring (HBPM) | Convenient for long-term use; multiple readings in real-world conditions; improves patient involvement | Requires patient education; device must be validated; no automatic nighttime reading (with basic devices) |
For many, HBPM is more than a clinical tool; it provides peace of mind. Dan Knapp, a 77-year-old patient, found that home monitoring saved him an 80-mile drive to the clinic. "The whole process is incredibly user-friendly... Not all my readings are perfect, but when they're not, I know my care team will be on top of it," he says. His blood pressure improved dramatically, from an uncontrolled level to a healthy 125/69 mm Hg .
A 2024 qualitative study from Sweden found that for motivated patients, HBPM "increases security, and leads to better communication about blood pressure between healthcare personnel and patients." The study identified an overarching theme among users: "It's all about the feeling of security".
Patients appreciated the ability to track trends and understand how their body responds to daily life.
Home blood pressure monitoring represents a significant advancement in personalized healthcare. By providing a clearer, more comprehensive view of your blood pressure, it empowers you and your doctor to make smarter, more effective decisions about your health. When combined with a validated device, proper technique, and a strong partnership with your healthcare provider, HBPM is a simple yet powerful strategy for taking control of your cardiovascular health and reducing your long-term risks.
Important Disclaimer: Do not stop or change your blood pressure medications based on home readings without first consulting your healthcare team. If you notice consistent unusual readings, contact your professional provider for guidance.
Better Blood Pressure Control: Research shows that active self-monitoring can lead to significant reductions in systolic and diastolic blood pressure.
A study published in The Lancet found that participants who monitored their blood pressure at home achieved greater reductions than those who received standard care .
Enhanced Patient Engagement: Taking measurements at home encourages individuals to become more active participants in their health, leading to better adherence to medication and lifestyle changes .
Informed Treatment Decisions: With a more complete data set, healthcare providers can make more precise adjustments to treatment plans, potentially helping patients reach their blood pressure goals faster .
Get the Right Cuff Size: A poorly fitting cuff is a common source of error. Measure the circumference of your upper arm and choose a cuff size accordingly. The cuff's bladder length should be 75% to 100% of your arm's circumference .
Position Your Arm Correctly: Place the cuff on your bare upper arm. Rest your arm on a table so that the cuff is at the same level as your heart .
Timing and Frequency: The standard protocol is to take two readings in the morning (before breakfast and medication) and two in the evening (before dinner), for at least 3 to 7 consecutive days.